There are at least three important reasons why Universal Health Coverage is urgently needed.
1. 1. Lack of access to health care for millions of poor, vulnerable, and marginalized people
According to WHO, at least half the world’s population is not covered by essential health services. Of the women who die in childbirth, 99% are in developing countries, and children are 14 times more likely to die before the age of five in sub-Saharan Africa. Communicable diseases, such as HIV, tuberculosis (TB) and malaria have the worst impact on the poorest and most marginalized communities. In all countries—whether low-, middle- or high-income—wide health gaps remain between the rich and poor. Weak health systems account for many of these gaps, highlighted and made worse by the COVID-19 pandemic.
Key Fact
UHC reforms have been a powerful driver for improving women’s health in several low- and middle-income countries, including Afghanistan, Mexico, Rwanda and Thailand. For more details see ‘Improving Women’s Health through Universal Health Coverage’.
2. Health costs push millions into poverty
In most countries worldwide, people have to pay for health-care services, which is one of the main reasons people fall into poverty. Many people with limited income, who must already make difficult choices between essential items and services, are forced to forgo the care they need.
Each year, more than 800 million people spend over 10% of their household income on health—this is known as catastrophic health spending. Of these, almost 100 million people a year are driven into extreme poverty (living on less than $1.25 per day) due to health care expenses. At the current pace, up to one-third of the world’s population will be in this situation in 2030.
Key Fact
In Thailand, UHC reforms led to a sharp reduction in the number of low-income families facing catastrophic expenditure within six years. For more information, see ‘Attaining UHC: A research initiative to support evidence-based advocacy and policy-making’.
3. Good health lifts people out of poverty
Good health allows children to learn and adults to earn, helps people escape from poverty, and provides the basis for long-term economic development.
Many global health challenges stem from a shared obstacle: under-resourced, fragile health systems that fail to provide the poorest and most marginalized communities access to quality, affordable health services. These gaps threaten lives and livelihoods, exacerbate rising inequality, and undermine economic growth and social stability in developed and developing countries alike. As crises like COVID-19 and Ebola have made painfully clear, our health systems are only as strong as their weakest links.
Countries implementing health systems strengthening and UHC policies are seeing the benefits: healthier communities and stronger economies.
Key Fact
It has been estimated that every $1 that a country invests in health today can produce up to $20 in full-income growth within a generation. For more, see ‘The Lancet Commission on Investing in Health’.
How UHC Supports the Wider SDGs
Besides contributing to SDG 3 (Ensure healthy lives and promote well-being for all at all ages) and SDG1 (End poverty in all its forms, everywhere), UHC can make a significant contribution to many of the other SDGs.
UHC promotes improved nutrition (SDG2)—nutrition-related interventions are a core part of comprehensive health benefit packages, and people receive more access to information and resources to address malnutrition. Strong health systems support educational goals (SDG4) because more children are healthy enough to attend school and families can afford schooling and gender equality (SDG5), by ensuring women and girls receive the necessary services they need. UHC also can play an important role in economic growth (SDG8), and peaceful and inclusive societies (SDG16), as healthy populations help build effective, accountable and inclusive institutions at all levels.
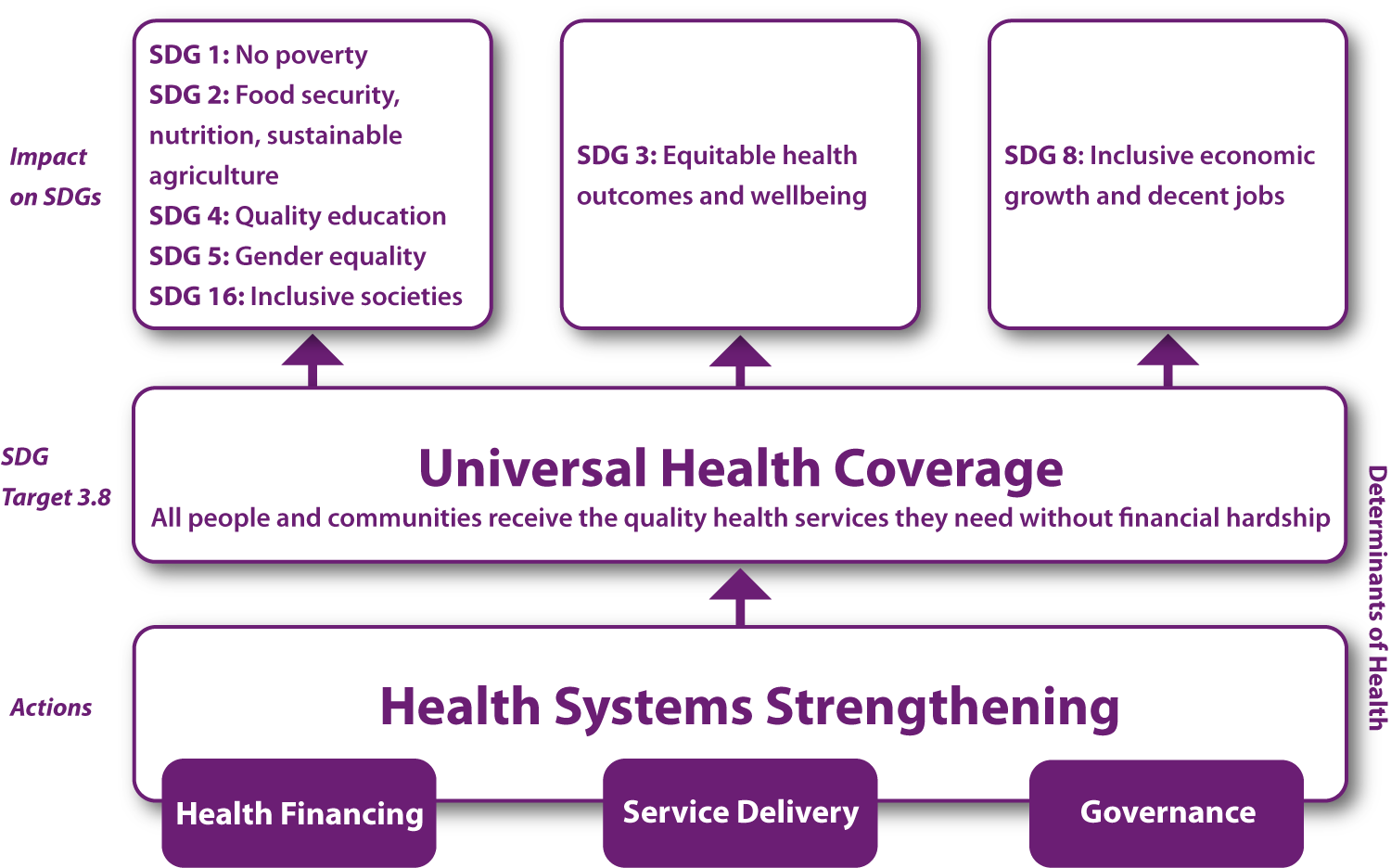
Universal health coverage is fundamental for achieving the Sustainable Development Goals not only to ensure health and well-being, but also to eradicate poverty in all its forms and dimensions, ensure quality education, achieve gender equality and women’s empowerment, [and] reduce inequalities. – UN Political Declaration on UHC, 2019
Lessons from COVID-19
The COVID-19 pandemic has clearly shown the linkages between health systems, emergency preparedness, and economic development, exposing major weaknesses and lack of investment in many of the world’s health systems.
To protect the health of their citizens and in efforts to prevent health systems from becoming overwhelmed, governments have had to implement drastic strategies, such as lockdowns and curfews. The pandemic and these response strategies have negatively affected the livelihood and well-being of all people, especially marginalized and vulnerable population groups including those with disabilities, and widened existing gaps in access to health.
Global health security is threatened by a lack of political will and investment in UHC. With deep economic recessions in lower-income countries due to COVID-19, health budgets are likely to be hit more than during the 2008 economic crisis. According to the recent Global Health Expenditure report, countries with health systems that depend on out-of-pocket payments are likely to be among those worst hit by the macro-economic impacts of the pandemic—lowering their public spending even further.
In addition, the consequences of COVID-19 on affected individuals, including the long-term physical impacts and financial burdens, and the consequences of disruptions to other health services, are still not fully understood. While the focus in most countries is still on immediate emergency response, it would be an error to consider moving back to business as usual and miss the opportunity to analyse the political and policy failures that have contributed to the severe impact of the COVID-19 pandemic.
Key Resource
For more information on the links between COVID-19 and UHC, see the CSEM paper on health and economic impacts of COVID-19 containment strategies.

